I am pretty sure you will have
read about or even
seen the
lecture by Karin Michels, the director of the
Institute for Prevention and Tumour Epidemiology at the
Albert-Ludwigs-University in Freiburg, Germany, which probably got so much attention, because Prof. Michels also works as an epidemiologist at the
Harvard TH Chan School of Public Health. In her lecture, she claims that there was no single clinical human study that would refute her claim that coconut oil (CO) was, due to its high concentration of saturated fatty acids (SFA), "pure poison" that would unquestionably "clog your arteries and lead to certain cardiovascular death" (translated based on the
video).

Protein Oxidation an Issue W/ High PRO Diets?

CHO ↓ = Perfor-mance ↓ - What about Avg. Joes?

More Protein ≠ More Satiety, Study Shows

Is Low Carb Even Crossfit Compatible?

Coffee Promotes Ketosis Despite High Carb Intakes

Keto Diet per se for Superior Weight Loss?
Now, while Michels is right when she says that
coconut oil is (over-)hyped and has been shown to negatively affect coconut lover's blood lipids (see 5 studies in the latter part of this articles), her claim that there was not a single study suggesting the safety, let alone health benefits of coconut oil is easy to falsify. Does that make coconut oil the "superfood" many people believe it was? Well, let's take a closer look at a dozen randomized clinical trials and decide then.
➪ Five exemplary studies that refute Michels' "there are no human studies"-claim:
 |
Figure 1: Fatty acid composition of popular
fats/oils (Wikipedia 2015) |
First, a comparative 90-day study by Nagashree et al. (2017) tested the effects of consuming 100g/day of coconut (CO | 91% SFA) vs. peanut oil (PO | 19% SFA) in 58 healthy volunteers and found "no significant deleterious effect on erythrocytes or lipid-related factors compared to groundnut [=peanut]] oil consumption", but "an increase in the anti-atherogenic HDL levels and anti-inflammatory precursor DGLA in erythrocyte lipids" (ibid.) of the CO group.
What has to be said, however, is that the LDL levels in the CO group increased, as well - and yes, elevated LDL alone is a marker CVD risk, not the only one (Field 2018) and maybe even not the best one (Yetley 2017), but the association of high LDL and cardiovascular disease is real. And, what's also important, the positive observation that there was no increased incorporation of the "pure[ly] poison[ous]" saturated fats into red blood cells tells us nothing about what happened in the walls of the arteries over the course of the 90-days study period and (obviously) beyond. Michels would thus probably argue that this comparison of a hard to a liquid fat (which is the main criterion Michels provides her audience when it comes to deciding whether an oil/fat can even be good for them), didn't properly assess potential increases in atherosclerotic plaque.
No, coconut oil does not cure Alzheimer's: It's claims like "coconut oil cures Alzheimer's" which are at least partly responsible for the bad reputation coconut oil has among scientists. Why? Well, as far as the cognitive enhancement claims are concerned, Michels is right: There are
no convincing human studies that would prove either general
cognitive improvements or alleviations of
Alzheimer's-induced cognitive decline.
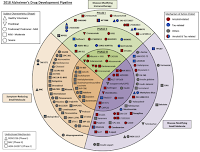 |
| The mere number of candidate drugs in Cummings latest (2018) illustration of the "Alzheimer's drug development pipeline" is impressive. The caprylic acid products AC-1202 and AC-1204 are yet no longer actively investigated - the industry's fault? I don't think so: Nestlé and other global players are invested in their producer Accera. |
The non-case-report human studies which are usually cited to support the putative cognitive improvements (e.g.
Reger 2004;
Henderson 2009) used "a product comprising predominantly of
caprylic acid (C8:0), one of the more minor fatty acids in coconut oil (present at around 7%)" (
Lockyer 2016). To simply assume that coconut oil would do the same as these purified oils (>95% caprylic acid is unwarranted.
What's also noteworthy is the fact that the product from the Henderson study, called AC-1202, has meanwhile been abandoned by its producer Accera, which (you guessed it) happens to be the employers of Henderson et al. Moreover, its successor AC-1204 (same mechanism)
has only recently failed to produce results in a well-powered phase 3 trial (
Cummings 2018). Accordingly, the "Alzheimer's claim" must, as of now, be considered part of the myth Michels rightly criticizes; and it'll remain a myth unless future studies prove her wrong.
- Second, a comparative 2-year study from India (Vijayakumar 2016) investigated the differential health effects of using coconut oil (CO | 91% SFA) versus sunflower oil (SFO | 12% SFA) on cardiovascular risk factors in 100 (final analysis n = 98) patients with stable coronary heart disease (CAD), i.e. a sub-group of the population the members of which are much more likely to actually die from consuming the "wrong" oils.
 |
| Table 2: Next to its superior duration, the fact that the scientists also measured the APO-B/A ratio is a major strength of Vijakumar et al's study - both is more or less unique in the literature (Vijakumar 2016). |
The scientists interpret the result, i.e. that there was "no statistically significant difference in the anthropometric, biochemical, vascular function, and in cardiovascular events after 2 years" as follows: "Coconut oil even though rich in saturated fatty acids in comparison to sunflower oil when used as cooking oil media over a period of 2 years did not change the lipid-related cardiovascular risk factors and events in those receiving standard medical care" (Vijayakumar 2016).
Plus: The study is a follow-up to an observational study by the same authors (Palazhy 2012), which assessed the fatty acid composition in habitual coconut vs. sunflower oil consumers' plaques by HPLC and didn't find significant inter-group differences between CAD patients who used CO vs. SFO, habitually.
Overall, the Vijaykumar studies come pretty close to the evidence of which Michels says that it doesn't exist. Plus: Unlike the previously discussed study by Nagshree et al., Palazhy et al. actually measured the plaque in the arteries, and the Vijayakumar study tracked the subjects' health for an impressive 2-years and measured not just total cholesterol, LDL, and HDL, but also the APO-B/A ratio, which has been proposed to "have better predictive value than that of classical lipid parameters in cardiovascular risk assessment" (quote from Tamang 2014; more info about in Hong 2015).
- Third, an RCT (Khaw 2018) that was conducted for the BBC show "Trust Me I'm a Doctor" compared the effects of consuming 50g/d virgin coconut oil (VCO) to extra virgin olive oil (EVOO), or butter (BT) for 4 weeks in 91 (initially 94) men and women. The results of this RCT directly contradict Michel's implicit claim that 'all saturated fats were alike' and all were 'evil' as it found that...
"[...] the effects of different dietary fats on lipid profiles, metabolic markers and health outcomes may vary not just according to the general classification of their main component fatty acids as saturated or unsaturated but possibly according to different profiles in individual fatty acids, processing methods as well as the foods in which they are consumed or dietary patterns" (Khaw 2018).
More specifically, the scientists found no worsening of LDL with virgin coconut oil (but with butter), and identical LDL levels in the VCO and EVOO groups, an improvement of HDL that was only observed in the VCO group, as well as a lack of effects on the important TC/HDL-C ratio and non-HDL-C ratios, which, you guessed it, deteriorated in the butter group.
 |
| Table 1: Mean changes in variables between baseline and follow-up after dietary interventions and pairwise comparisons between fats in 91 participants (Khaw 2018). |
Now, this isn't just one of the allegedly non-existing studies that confirm the safety of coconut oil, but also one of the few that actually suggests health benefits over a fat Prof. Michels included on her "even ... is better than coconut oil"-list: butter. Furthermore, the results of Khaw's study emphasize that there's a "need for further elucidation of the more nuanced relationships between different dietary fats and health" (Khaw 2018) - a nuance Prof. Michels either doesn't know about or - which is more likely - preferred to ignore in her lecture.
Coconut oil is also not identical to MCT oil! Often coconut lovers refer to studies investigating the effects of MCT oils to prove the alleged benefits of coconut oil. With an average MCT content of "only" 45-53% coconut oil is yet not pure MCT and we cannot simply assume that it will cause the same beneficial effects as "pure" medium-chain-triglyceride oils (e.g. curb appetite |
Kinsella 2017).
- Fourth, an intervention trial by Cardoso et al. (2015) investigated the effects of consuming additional 13 g/d of extra virgin coconut oil (>12 g SFA, per serving) would have on the anthropometric parameters and lipid profile of older patients (45-85 years old) with coronary artery disease (CAD), who consumed a standardized diet that was optimized for individuals with dyslipidemia.
The study had two phases: In phase 1 intensive care phase (0-3 months), in which all subjects received the same diet and lost significant amounts of weight, and the second phase, in which half of the n=161 subjects supplemented with 13ml/d of extra virgin coconut oil (the other subjects didn't receive extra-fats). In this second phase lasting from month 3 to month 6, the scientists observed a sign. more pronounced further decrease in waist circumference (-2.1 cm vs. -0.1cm in EVCO vs. no supplement).
 |
| Figure 2: The additional extra virgin coconut oil (EVCO) had surprisingly beneficial effects (A) on the waist circumference in the 2nd phase of Cardoso's study. The increase in HDL (B), on the other hand, was expected, because numerous previous studies have shown increases in HDL w/ coconut oil. |
The progressive reduction of the subjects' waist circumferences in the Cardoso study clearly suggests reductions in visceral fat. In conjunction with the significantly improved HDL levels (+3.1 mg/dL vs. -1.2 mg/dL in EVCO vs. no supplement), this response to the addition of EVCO to the diet is not just another item on the list of the allegedly non-existing studies in favor of cardiovascular health benefits of coconut oil, but can actually be seen as evidence in favor of coconut oil's superfood status.
- And last, but not least, fifth, a very recent study by Oliveira-de-Lira et al. (2018) that compared the effects of 8 weeks on hypocaloric diets supplemented (pre-meal) with coconut oil (CO | here 93% SFA), safflower oil (SAF | here 5% SFA), and chia oil (CHIA | here 14% SFA) and compared them to a control condition, in which the subjects, seventy-five overweight/obese women consumed soybean oil (SOY | here 20% SFA), instead. The subjects' weight, anthropometric parameters, and body fat (%BF), as well as their lean mass percentages (%LM), were evaluated along with biochemical parameters related to lipid and glycemic profiles before and after the 8-week intervention.
 |
| Figure 3: Relative changes (%) in body weight (left) and body fat (right) over the course of the 8-week study by Oliveira-de-Lira et al. according to type of fatty acid suppl.; * p<0.05 vs. CHIA & SOY; ** p<0.05 for SOY. |
And guess what, the subjects who consumed 3x2g of CO 30 minutes before meals (a) lost the most weight and body fat (p < 0.05 vs. CHIA and SOY for both, %weight and %body fat | see Figure 3) and gained the highest amount of %lean mass (2.61% ± 1.40 kg, p < 0.001 for pre- vs. post and p < 0.05 vs. CHIA and SOY).
Cool? Well, the improvements in body composition are nice, but the results that will bother Prof. Michels are different ones: the scientists also found that the coconut supplement had the most pronounced beneficial effect on the long-term glucose gauge HbA1c (-0.86% vs. -0.49%, -0.53%, and -0.36% in the SAF, CHIA, and SOY group, respectively). With elevated HbA1c being in itself a risk factor for cardiovascular disease (Singer 1992; Selvin 2005 & 2006), this could be interpreted as yet another indicator of health-benefits of coconut oil - one that has been observed in direct comparison to high MUFA and PUFA oils, of which Michelsen is convinced that they are much healthier than coconut oil.
As far as the mechanism is concerned, we can by the way, exclude that the benefits were a mere results of the ~100kcal greater reduction in energy intake in the coconut group (−612.69 kcal/day in the CO group vs. -500.49, -532.59, and -532.50 kcal/day in the SAF, CHIA, and SOY group respectively). Accordingly, something else must be responsible for the observed benefits on body composition and glycemia, and the scientists' observation that total cholesterol, LDL, VLDL, and triglycerides changed in response to CO to the same extent as they did in the SAF and SOY treatments, while HDL increased just as much in the CO group as it did in the CHIA group, which produced the highest reductions in total and LDL cholesterol.
➪ Two studies showing no clear results:
- Two studies by Cox et al. (1995 & 1998) compared the health effects of the consumption of coconut oil (CO) to safflower (SAF) and butter (BT) in 28 subjects (Cox 1995) and 41 healthy Pacific Island Polynesians (Cox 1998), respectively. In the 1995 and 1998 study, subjects consumed 50% and 46% of their total fat intake in form of CO, SAF, or BT, respectively.
|
|
| Figure 4: Lipid levels in Cox 1998 relative to the allegedly healthy PUFA alternative Safflower oil | I've marked all changes that must be considered negative w/ (-) and all those which must be considered positive w/ (+). |
What the scientists found is not exactly surprising: In the 1995 study, butter increased total (TC) and LDL cholesterol significantly more than coconut oil, which, in turn, produced significantly higher TC and LDL levels than the safflower oil - the absolute differences are yet 0.4 mmol/L for BT > CO and 0.3 mmol/L for CO > SAF and thus not exactly huge. Moreover, HDL increased significantly only on the high SFA diets, i.e. BT and CO - albeit only in women.
In the 1998 study (see Figure 4), the results were not much different. More specifically, butter takes the lead for both total cholesterol and LDL, with coconut oil showing sign. lower LDL levels than butter, but significantly higher LDL levels than safflower oil. For all other lipid parameters, however, coconut oil showed a more heart-friendly lipid profile - statistical significance was yet achieved only for HDL, but not for VLDL and triglycerides (TG). In view of the fact that the apolipoprotein B/A ratios for the three treatments were 0.81, 0.65, and 0.66 for BT, CO, and SAF, respectively, it is difficult to say whether coconut oil is, in fact, less heart-healthy for Pacific Islanders than safflower oil... with the LDL levels remaining well within the normal zone and the identical APO-ratio, one could argue that it's not, which is why I didn't assign this study to either the pro- or anti-coconut oil evidence.
➪ Five studies supporting Michels' claims about CO's neg. effect on blood lipids:
- A study with a somewhat unique design by Ng et al. (1991) assessed the effects of diets supplying ∼75% of the fat calories from coconut oil (CO | here SFA 75.1%), palm olein (PO | here SFA 45.6%), and corn oil (CORN | here SFA 30.4%) in three 15-week dietary periods using three matched groups of healthy volunteers (61 males, 22 females, aged 20–34 y): the CO - PO - CO, the CO - CORN - CO, and the CO - CO - CO group (note: the CO - PO - CO group, for example, would consume CO for five weeks, PO for five weeks, and CO for five weeks).
 |
| Table 3: Serum total cholesterol responses by sex in at the end of periods II and III (Ng 1991). |
Based on Prof. Michels' method of rating dietary fats/oils only based on their saturated fat (SFA) content, the outcomes should be CORN > PO > CO in terms of heart healthiness. And guess what!? That was exactly what the scientists found. Coconut oil produced persistently the highest total cholesterol and LDL levels (CO > PO > CORN) and even though the HDL concentration was slightly higher in the CO-phases, the important LDL/HDL ratio was significantly lower for CORN vs. CO and non-significantly lower for PO vs. CO. No clear effect was observed for triglycerides.
A 2011 study by Voon, Ng, and Nesaratam, of which one could argue that it was the late "follow up" to the 1991 paper also support Michels' conviction. The study investigated the effects of high-protein Malaysian diets prepared with palm olein (PO | here 12.5%E SFA), coconut oil (CO | here 20.6%E SFA), or virgin olive oil (VOO | here 6.6%E SFA) on plasma homocysteine and selected markers of inflammation + cardiovascular disease (CVD) in 45 healthy adults over 3x5-week periods. What makes this follow-up interesting is that it (a) used everybody's darling, virgin olive oil, as one of the control oils, and (b) went beyond measuring only changes in blood lipids.
Why's that interesting? Well, while lipids increased as usual (with CO > PO > VOO for total cholesterol, triglycerides, LDL, and HDL) both the identical total/HDL cholesterol ratios and the lack of a difference in markers of inflammation, i.e. homocysteine, TNF-α, IL-1β, IL-6, and IL-8, high-sensitivity C-reactive protein, and interferon-γ, put at least a small question-mark behind the notion that coconut oil is the killer Michel says it is.
- Two studies by Mendis et al. (1990 & 2001) also found the obvious increases in blood lipids in a coconut (CO) vs. soybean oil (SOY) group... anyway, let's be a bit more specific: In their study from 1990, Mendis et al. put twenty-five young normolipidemic males on isoenergetic diets containing 30% of energy as fat (70% of the total fat coming from CO and SOY, respectively) for 8 weeks (Mendis 1990). The scientists calculated the PUFA:SFA-ratio of the test diets to be 0.25 for the coconut oil diet and 4 for the soybean oil diet.
In view of the results of the previously discussed studies, no one should be surprised that the 1990 study observed significant increases in total cholesterol (+25%), LDL (+25%), HDL (+15%) and triglycerides (+25%) in the CO group (vs. SOY).
In the "follow-up" (Mendis 2001), the scientists from the WHO in Switzerland investigated the effects of replacing saturated fats from coconut oil (CO) with unsaturated fats from soybean oil (SOY) and sesame oil (SESAM). The study had two phases with phase 1 testing the effects of decreasing the PUFA/SFA ratio of the standardized high saturated fat (SFA) diet all subjects had received in the lead-in (17.8% of the total energy from CO) from 0.4 to 0.2 by reducing both the total fat and coconut oil (now 9.3% of the energy) in the subjects diets.
 |
| Table 4: Mean daily intake of energy and nutrients of subjects in Mendis 2001. |
The 52-week-long 2nd phase, is not of interest to us, because the amount of coconut oil in the diets is so low (4.7%) that it's just another SFA vs. PUFA study unable to give us any relevant information about the health effects of specific saturated/unsaturated fats/oils.
 |
| Figure 5: Serum values (mmol/L) of total cholesterol, LDL-C, HDL-C and triglyceride levels, as well as the total:HDL cholesterol ratio and relative changes (in %) when switching from a high-SFA diet w/17.8% of the energy from coconut oil to a lower-SFA diet w/ only 9.3% of the energy from coconut oil (Mendis 2001). |
If you take a look at what happened in phase I (Figure 5), when the subjects switched from a high coconut (17.8%) to a lower (9.3%), you will see that only total and LDL cholesterol decreased significantly in response to the (methodologically questionably) reduction of both total fat and the contribution of coconut oil to the total energy intake (see Table 4). In terms of triglycerides (TAG) and the total:HDL cholesterol ratio, only a non-significant advantage for the low coconut oil diet was observed. The overall effect of higher amounts of CO in the diet must still be rated as rather detrimental - that doesn't change the fact, though, that the methodology of the study is not really suited to objectively single out the effects of coconut oil.
- Not lard, but beef fat was the object of a study by Reiser et al. from 1985 that evaluated the fasting human plasma lipid and lipoprotein responses to dietary beef fat (BF) vs. coconut oil (CO), or safflower oil (SAF). A study with the results you'd expect: The nineteen free-living normolipidemic men (aged 25.6 +/- 3.5 yr) who consumed prepared lunches and dinners containing 35%E total fat, 60% of which was the test fat, for five weeks saw significantly higher total (TC), and HDL cholesterol levels in the CO compared to both, the BF and SAF weeks.
 |
| Figure 6: Lipid levels in (mmol/L) after 5 weeks on diets containing 18% of the total energy as beef fat (BF), coconut oil (CO), and safflower oil (SAF) - the pre-prepared diets (lunch + dinner) were administered subsequently in a random order w/ 5 weeks on the habitual diet between the treatments (Reiser 1985). |
What is interesting, though, is that the outcome for LDL and triglycerides were slightly different: While the CO diet produced the highest LDL levels, the difference was significant only compared to the SAF, but not the beef fat diet. The same diet that also produced the highest levels of triglycerides (see Figure 5 for the exact lipid levels and p-values).
In spite of the lack of significance compared to beef fat, the study still supports Michels' position. After all, the high PUFA oil came out victorious and beef fat was (just as Michels claims it in her lecture for lard) less harsh on all but one blood lipid level than coconut oil.
If you've gotten to this point, you will probably already have formed your own (now educated) opinion. If you're still interested in mine, just continue reading the bottom line.
So, is Prof. Michels right? Unfortunately, there's no clear answer to this question.
Unwarranted claims: She is
clearly wrong when she says that there were
no human studies which suggest beneficial health effects of coconut oil. In this article, I've discussed five exemplary studies (+ related evidence), in which coconut oil had either identical or even superior effects on subject health and/or body composition compared to both, other high-saturated fat, such as butter, as well as low-saturated-fat oils, such as
peanut oil,
sunflower oil, and even
olive oil.
She is
also wrong when she says that
you can judge the health-properties of an oil based on its saturated fat content, let alone its phase of matter at room temperature (liquid = good vs. solid = bad). Butter, for example, is much softer than coconut oil at room temperature and still got away much worse than coconut oil in all studies which actually compared the two "solid" high-SFA fats.
 |
| The whole "coconut oil debate" shares the same short-sighted over-generalizations as the debate about red meat, where all forms of red meat (processed & unprocessed, cured and salted or fresh, etc.) are lumped together into one big bad "red meat" category and differences such as those between high-SFA fats like butter and coconut oil are ignored | more |
Warranted claims: On the other hand,
Prof. Michels is right, when she says that
there are numerous human studies showing negative effects of coconut oil on blood lipids when it is compared to lower-SFA oils. And, since
she's also right when she highlights that
the corresponding increase in LDL has been consistently linked to an increase in heart disease risk, it would be unwarranted to conclude that coconut oil was the best oil for our heart health.
In that, it can yet hardly be overemphasized that this conclusion is fundamentally different from calling coconut oil "pure poison" based on studies, of which a 2016 review by
Eyres 2016 says that they have "important limitations" - including small sample sizes, biased samples, inadequate dietary assessments, and a strong likelihood of confounding.
The verdict: In short, coconut oil is
not pure poison. Studies suggesting
beneficial metabolic effects and the
cardiovascular safety of coconut oil
do exist. The lipid-elevating effects of coconut oil are still undeniable and more research with robust disease outcomes (not just blood lipids and other CVD risk markers |
Eyres 2016;
Lockyer 2016) is necessary to find out if copious amounts of coconut and virgin coconut oil increase our real-world risk of cardiovascular disease. In the meantime, I, personally, won't throw away my jar of virgin coconut oil, but keep it in the rotation with olive oil and high MUFA rapeseed oil - a mix that yields stable, low LDL levels for me (
warning: do not simply assume it's the same for you) |
Comment!
References:
- Cardoso, Diuli A., et al. "A coconut extra virgin oil-rich diet increases HDL cholesterol and decreases waist circumference and body mass in coronary artery disease patients." Nutricion hospitalaria 32.5 (2015).
- Cox, C., et al. "Effects of coconut oil, butter, and safflower oil on lipids and lipoproteins in persons with moderately elevated cholesterol levels." Journal of lipid research 36.8 (1995): 1787-1795.
- Cox, C., et al. "Effects of dietary coconut oil, butter and safflower oil on plasma lipids, lipoproteins and lathosterol levels." European journal of clinical nutrition 52.9 (1998): 650.
- Cummings, Jeffrey, et al. "Alzheimer's disease drug development pipeline: 2018." Alzheimer's & Dementia: Translational Research & Clinical Interventions (2018).
- Field, Patrick A., and Ramachandran S. Vasan. "LDL‐Cholesterol Is Not the Only Clinically Relevant Biomarker for Coronary Artery Disease or Acute Coronary Syndrome." Clinical Pharmacology & Therapeutics (2018).
- Dayrit, Fabian M. "The properties of lauric acid and their significance in coconut oil." Journal of the American Oil Chemists' Society 92.1 (2015): 1-15.
- Henderson, S. T., et al. "Study of the ketogenic agent AC-1202 in mild to moderate Alzheimer's disease: a randomized, double-blind, placebo-controlled, multicenter trial." Nutrition & metabolism 6 (2009): 31.
- Hong, Li-Feng, et al. "Is the ratio of apoB/apoA-1 the best predictor for the severity of coronary artery lesions in Chinese diabetics with stable angina pectoris? An assessment based on Gensini scores." Journal of geriatric cardiology: JGC 12.4 (2015): 402.
- Kaushik, Mamta, et al. "The effect of coconut oil pulling on Streptococcus mutans count in saliva in comparison with chlorhexidine mouthwash." J Contemp Dent Pract 17.1 (2016): 38-41.
- Khaw, Kay-Tee, et al. "Randomised trial of coconut oil, olive oil or butter on blood lipids and other cardiovascular risk factors in healthy men and women." BMJ open 8.3 (2018): e020167.
- Kinsella, R., T. Maher, and M. E. Clegg. "Coconut oil has less satiating properties than medium chain triglyceride oil." Physiology & behavior 179 (2017): 422-426.
- Lockyer, S., and S. Stanner. "Coconut oil–a nutty idea?." Nutrition Bulletin 41.1 (2016): 42-54.
- Lyte, Joshua M., Nicholas K. Gabler, and James H. Hollis. "Postprandial serum endotoxin in healthy humans is modulated by dietary fat in a randomized, controlled, cross-over study." Lipids in health and disease 15.1 (2016): 186.
- Mendis, Shanthi, and Ravi Kumarasundaram. "The effect of daily consumption of coconut fat and soya-bean fat on plasma lipids and lipoproteins of young normolipidaemic men." British Journal of Nutrition 63.3 (1990): 547-552.
- Mendis, Shanthi, U. Samarajeewa, and R. O. Thattil. "Coconut fat and serum lipoproteins: effects of partial replacement with unsaturated fats." British Journal of Nutrition 85.5 (2001): 583-589.
- Oliveira-de-Lira, Luciene, et al. "Supplementation-Dependent Effects of Vegetable Oils with Varying Fatty Acid Compositions on Anthropometric and Biochemical Parameters in Obese Women." Nutrients 10.7 (2018).
- Palazhy, Sabitha, et al. "Composition of plasma and atheromatous plaque among coronary artery disease subjects consuming coconut oil or sunflower oil as the cooking medium." Journal of the American College of Nutrition 31.6 (2012): 392-396.
- Pastori, Daniele, et al. "Gut‐Derived Serum Lipopolysaccharide is Associated With Enhanced Risk of Major Adverse Cardiovascular Events in Atrial Fibrillation: Effect of Adherence to Mediterranean Diet." Journal of the American Heart Association 6.6 (2017): e005784.
- Reger, Mark A., et al. "Effects of β-hydroxybutyrate on cognition in memory-impaired adults." Neurobiology of aging 25.3 (2004): 311-314.
- Reiser, Raymond, et al. "Plasma lipid and lipoprotein response of humans to beef fat, coconut oil and safflower oil." The American journal of clinical nutrition 42.2 (1985): 190-197.
- Selvin, Elizabeth, et al. "Glycemic control and coronary heart disease risk in persons with and without diabetes: the atherosclerosis risk in communities study." Archives of internal medicine 165.16 (2005): 1910-1916.
- Selvin, Elizabeth, et al. "HbA1c and peripheral arterial disease in diabetes: the Atherosclerosis Risk in Communities study." Diabetes care 29.4 (2006): 877-882.
- Singer, Daniel E., et al. "Association of HbA1c with prevalent cardiovascular disease in the original cohort of the Framingham Heart Study." Diabetes 41.2 (1992): 202-208.
- Tamang, Hem Kumar, et al. "Apo B/Apo AI ratio is statistically a better predictor of cardiovascular disease (CVD) than conventional lipid profile: a study from Kathmandu Valley, Nepal." Journal of clinical and diagnostic research: JCDR 8.2 (2014): 34.2
- Vijayakumar, Maniyal, et al. "A randomized study of coconut oil versus sunflower oil on cardiovascular risk factors in patients with stable coronary heart disease." Indian Heart Journal 68.4 (2016): 498-506.
- Voon, Phooi Tee, et al. "Diets high in palmitic acid (16: 0), lauric and myristic acids (12: 0+ 14: 0), or oleic acid (18: 1) do not alter postprandial or fasting plasma homocysteine and inflammatory markers in healthy Malaysian adults–." The American journal of clinical nutrition 94.6 (2011): 1451-1457.
- Yetley, Elizabeth A., David L. DeMets, and William R. Harlan Jr. "Surrogate disease markers as substitutes for chronic disease outcomes in studies of diet and chronic disease relations." The American journal of clinical nutrition 106.5 (2017): 1175-1189.






















