Iodine Induced Reduction in Hepatic Deiodinase Activity Leads to Hypothyrodism and the Accumulation of Liver Fat That May Eventually Pave the Way to Diabesity
The Ying and Yang of high and low iodine intake
A recently published rodent study from the Huazhong University of Science and Technology, the Binzhou Medical University and the Shen Zhen Center for Chronic Disease Control, in China (Xia. 2013) does now shed some light onto the underlying mechanisms of the well-known thyroid disrupting effects of the structural backbone of all mammalian thyroid hormones, iodine. While the whole spectrum of disorders of iodine excess includes hypothyroidism, hyperthyroidism, autoimmune thyroiditis,embryo toxicity, and depression of brain development (Guo. 2006; Rose. 2001; Roti. 2001; Yang. 2006) Yun Xia et al. are probably the first to investigate its hazardous effects of iodine excess on the liver.
To this end, the Chinese researchers supplemented rats on a standard diet containing a baseline level of 365μg/kg iodine with different doses of iodine in the form of potassium iodate (KIO3) in the drinking water for 3 months:
"In 2000, the Chinese Nutrition Society stated that the recommended nutrient intake (RNI) of iodine of adults is 150μg/day and the tolerable upper intake level (UL) is 1,000μg/day.According to these results, the mice in the study were randomized to receiver either 0, 0.3, 0.6, 1.2, 2.4, and 4.8 mg I/L iodine, corresponding to 0-, 1-, 2-, 4-, 8-, and 16-fold of the adequate/normal iodine intake for 3 months to explore the dose-dependent effect of iodine on hepatic steatosis. In the course of the trial, dood consumption, water consumption of each group, were recorded meticulously and the weight gain of each mouse was recorded daily.
Conversely, intake of iodine at about sixfold of its RNI may induce injury. In addition, many excess iodine animal experimental data indicate that ten times the normal iodine intake in mice for about 3 months can cause damage. Moreover,the results of our previous experiment show that drinking 1.2 mg I/L iodine water for 1 month had no significant effect on serum lipid metabolism, while prolonged exposure for 3 months induced an increase of serum cholesterol." (Xia. 2013)
Additionally, another 60 weaning female Balb/c mice were randomly assigned to six groups and given iodine at different levels (0, 0.3, 0.6, 1.2, 2.4, and 4.8 mg I/ml) for 1 month just for
measuring the oxidative stress parameters in serum and liver.
 |
| Figure 1: Triglyceride content in liver and serum, as well as SREBP-1c and fatty acid syntethase (FAS) activity after 3 months on diets with additional iodine (Xia. 2013) |
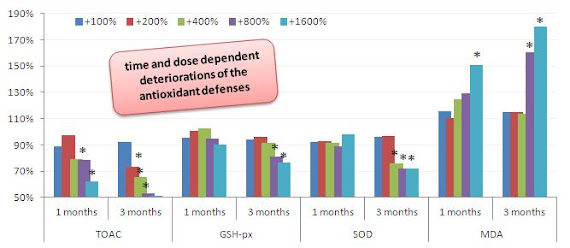 |
| Figure 2: Total antioxidant capacity, glutathione peroxidase, SOD, and lipid peroxidation (MDA) after 1 and 3 months expressed relative to untreated control (Xia. 2013) |
 |
| Figure 3: Changes in thyroid hormone and deiodinase levels; expressed. rel. to control (Xia. 2013) |
Low D1 => Low T3 => fatty liver disease
In fact, the reduced local conversion of T4 to T3, is also behind the accumulation of triglycerides in the liver and blood of the animals, as the
"[r]educed plasma T3 level resulted in the upregulation of SREBP-1c mRNA and FAS mRNA that ultimately led to the accumulation of triglycerides in the liver. [...] Evident hepatic steatosis was observed in mice challenged with 2.4 and 4.8 mg I/L iodine in drinking water. " (Xia. 2013)As a SuppVersity student you know about the downstream effects, but I guess it makes sense to reiterate them for the newbies: Since the liver plays a, if not the pivotal role in systemic lipid homeostasis the reduced oxidation of triglycerides and the increased storage will sooner or later lead to an increased secretion of triglyceride-rich lipoprotein (VLDL) as a compensatory response by which the liver will desperately try to spread the lipid burdon to other organs and tissues. Overwhelmed with the sudden onslaught of triglyceride laden VLDL particles which are easily oxidized during their voyage through your blood stream, this opens the door to a narrowing of the arteries, cardiovascular disease and stroke.
 |
| For the majority of you, overtraining and undereating is probably a much greater threat, when it comes to hypothyrodism (learn more about "self-inflicted hypothyrodism"). However, contrary to excess iodine intake that will not clog up your liver and arteries and eventually cause heart disease and stroke. |
Yet, although I would be cautious about extrapolating the exact cut-off levels, it appears that dietary intakes in the 800µg range and thus 4-6x more than the RDA can still be considered relatively save. So if you are neither taking high dose supplements or living on tons of seaweed, this is probably not much of a concern for most of you. In addition it would warrant investigation if / to which extent the addition of extra selenium would ameliorate these effects. After all, the latter has been shown to have protective effects against iodine intoxication in the very same rodent model in a 2006 study by Xu et al. (Xu. 2006).
References:
- Guo H, Yang X et al. Effect of selenium on thyroid hormone metabolism in filial cerebrum of mice with excessive iodine exposure. Biol Trace Elem Res. 2006; 113:281–295.
- Rose NR, Bonita R et al. Iodine: an environmental trigger of thyroiditis. Autoimmun Rev. 2002; 1:97–103.
- Roti E, Uberti ED. Iodine excess and hyperthyroidism. Thyroid. 2001;11:493–500.
- Xia Y, Qu W, Zhao LN, Han H, Yang XF, Sun XF, Hao LP, Xu J. Iodine Excess Induces Hepatic Steatosis Through Disturbance of Thyroid Hormone Metabolism Involving Oxidative Stress in BaLB/c Mice. Biol Trace Elem Res. 2013 May 28.
- Xu, J, Yang, XF., Guo, HL, Hou, XH Liu, LG, & Sun, XF. Selenium supplement alleviated the toxic effects of excessive iodine in mice. Biological trace element research; 2006 111(1-3), 229-238.
- Yang XF, Xu J et al. Developmental toxic effects of chronic exposure to high doses of iodine in the mouse. Reprod Toxicol. 2006: 22:725–730.
- Zhao J, Wang P, Shang L, Sullivan KM, van der Haar F, Maberly G. Endemic goiter associated with high iodine intake. Am J Public Health. 2000 Oct;90(10):1633-5.



