Pre-Hypertension Ain't Benign: Up to 80% Increased Risk of Cardiovascular Morbidity W/ "High Normal" Blood Pressure and Less! Plus: Foods & Supps to Reduce Your BP
 |
| "High normal" is misleading - there is no such thing as a "high normal" BP |
If that sounds familiar, it may be useful to show him a recent meta-analysis of pertinent papers from the early 2000s - a metapa-analysis like the one Yuli Huang and her colleagues from the Department of Cardiology at the Nanfang Hospital at the Southern Medical University in Guangzhou, China, published in BMC Medicine a couple of days ago (Huang. 2014).
"Pre-hyper-tensive? Pah that's not me!" If you just thought that,
I'd hope that you are right, but honestly... in view of the fact that 3
out of 10 US citizens have a blood pressure in the 129-139 / 84-95 mmHg
and against the background that the latter has long been considered as
"high normal" I am afraid that some of you may qualify for the
>50% increase in heart disease risk as a result of "suboptimal" blood
pressure values.
In said paper Huang et al. present the results of an extensive database search in the course of two independent reviewers identified 18 prospective cohort studies with a total of 468,561 participants the researchers used to evaluate the cardiovascular and coronary heart disease (CVD and CHD) risk in prehypertensive individuals. |
| Figure 1: Risk increases for cardiovascular morbidity (all subjects, left), stroke and cardiovascular heart disease (right); difference expressed relative to subjects w/ normal BP (Huang. 2014) |
If you look at the data, the Chinese researchers present in their latest paper, it turns out that even a blood pressure below what is usually considered "high normal", i.e. a systolic blood pressure between 130 and 139 in concert with a diastolic blood pressure of 85 to 89 mm Hg. In fact, Huang et al. report at statistically significant increase in cardiovascular morbidity of 46% even in those of the almost 5000,000 study participants with "below high normal" levels of 120-129 / 80-84 and thus in a BP range where your doctor may even say: "Hey that's pretty good!"
If you happen to be lucky enough to be a women, the risk will be slightly reduced. If, on the other hand, you are a man, your CVD morbidity risk will increase by 80% - irrespective of your age, by the way.
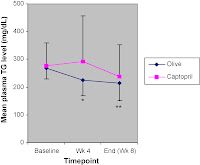 |
| Not on the list on the left, but in the SuppVersity News: " Olive Leave Extract Equally Effective at Lowering Blood Pressure as ACE Inhibitor Captopril" | read more |
Supplements that may be useful are taurine (Militante. 2002), fish oil (Campbell. 2013), dark chocolate / cacao (Desideri. 2012), vitamin C (short term; Juraschek. 2012), green tea extracts (Bogdanski. 2012), pomegrenate (Asgary. 2013; juice), melatonin (Scheer. 2004) and - as on every list of suggested supplements - whey protein (Lee. 2007) ;-)
- Asgary, Sedigheh, et al. "Clinical Evaluation of Blood Pressure Lowering, Endothelial Function Improving, Hypolipidemic and Anti‐Inflammatory Effects of Pomegranate Juice in Hypertensive Subjects." Phytotherapy Research (2013).
- Bogdanski, Pawel, et al. "Green tea extract reduces blood pressure, inflammatory biomarkers, and oxidative stress and improves parameters associated with insulin resistance in obese, hypertensive patients." Nutrition Research 32.6 (2012): 421-427.
- Campbell, Fiona, et al. "A systematic review of fish-oil supplements for the prevention and treatment of hypertension." European journal of preventive cardiology 20.1 (2013): 107-120.
- Desideri, Giovambattista, et al. "Benefits in Cognitive Function, Blood Pressure, and Insulin Resistance Through Cocoa Flavanol Consumption in Elderly Subjects With Mild Cognitive Impairment The Cocoa, Cognition, and Aging (CoCoA) Study." Hypertension 60.3 (2012): 794-801.
- Geleijnse, J. M., et al. "Reduction in blood pressure with a low sodium, high potassium, high magnesium salt in older subjects with mild to moderate hypertension." Bmj 309.6952 (1994): 436-440.
- Juraschek, Stephen P., et al. "Effects of vitamin C supplementation on blood pressure: a meta-analysis of randomized controlled trials." The American journal of clinical nutrition 95.5 (2012): 1079-1088.
- Kass, Lindsy, J. Weekes, and Lewis Carpenter. "Effect of magnesium supplementation on blood pressure: a meta-analysis." European journal of clinical nutrition 66.4 (2012): 411-418.
- Militante, J. D., and J. B. Lombardini. "Treatment of hypertension with oral taurine: experimental and clinical studies." Amino Acids 23.4 (2002): 381-393.
- Rosanoff, Andrea. "Magnesium supplements may enhance the effect of antihypertensive medications in stage 1 hypertensive subjects." Magnesium Research 23.1 (2010): 27-40.
- Scheer, Frank AJL, et al. "Daily nighttime melatonin reduces blood pressure in male patients with essential hypertension." Hypertension 43.2 (2004): 192-197.


